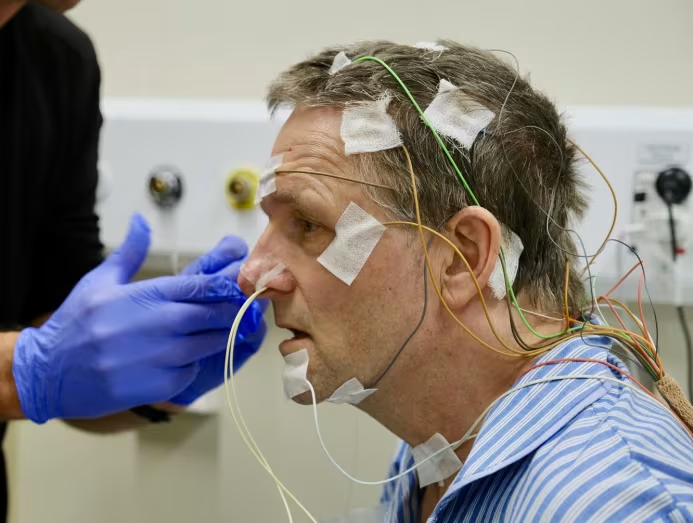
How Accurate Is Sleep Testing Australia for Detecting Sleep Issues?
What does “accuracy” mean in sleep testing?
In sleep testing, “accuracy” usually means how reliably the study identifies a disorder and grades its severity. They look for repeatable patterns in breathing, oxygen levels, brain activity (in lab studies), heart rate, and body movement. A test can be “accurate” for one condition like OSA, but less reliable for others like narcolepsy unless the right protocol is used.
Which types of sleep tests does Sleep Testing Australia typically use?
Sleep Test Australia providers typically offer home sleep apnoea testing (HSAT) and may facilitate in-lab polysomnography through partner clinics or referral pathways. HSAT is designed primarily to detect breathing-related sleep disorders, while in-lab polysomnography is broader because it records more signals, which helps when symptoms are complex or when non-breathing disorders are suspected.
How accurate are home sleep tests for obstructive sleep apnoea?
Home sleep tests are often quite accurate for moderate to severe OSA in people with a high likelihood of the condition. They measure airflow, breathing effort, and oxygen desaturation, which are key markers for OSA. Accuracy can drop for mild OSA, positional OSA, or when the equipment is worn incorrectly, because fewer signals are recorded than in a lab study.
When is an in-lab sleep study more accurate than a home test?
An in-lab study is more accurate when they need to measure sleep stages, arousals, limb movements, seizures, or unusual behaviours during sleep. It is also preferred when the person has significant comorbidities, suspected central sleep apnoea, or when prior home testing is negative despite strong symptoms. The added sensors reduce ambiguity and help rule in or rule out alternative diagnoses.
How much does sensor placement and user setup affect results?
Setup quality can materially affect accuracy, especially for home tests. If the nasal cannula shifts, the oximeter loosens, or the chest belt is mispositioned, the device may undercount breathing events or misread oxygen drops. Many services reduce this risk by providing clear instructions, fit-check guidance, and data-quality screening before a report is finalised.
Can sleep testing miss a real sleep problem?
Yes, they can miss an issue if the wrong test is used or if the condition is intermittent. Mild OSA can be missed if there are few events on that specific night, and some disorders require specialised tests beyond standard apnoea studies. A “normal” result should be interpreted alongside symptoms, history, and risk factors rather than treated as the only decision point.
How reliable are severity scores like AHI from these tests?
AHI is generally reliable when the signals are clean and the scoring rules are applied consistently. Home tests often estimate sleep time indirectly, which can slightly skew AHI compared with lab studies that measure actual sleep with EEG. That means they might under- or over-estimate severity in borderline cases, even if the overall diagnosis is still correct.
What should they do if results do not match symptoms?
They should discuss the outcome with a clinician and consider a repeat study or an in-lab polysomnography if suspicion remains high. They can also review whether the device data had artefacts or poor signal time. If symptoms include severe daytime sleepiness, sudden sleep attacks, or unusual night behaviours, they may need a different diagnostic pathway rather than another home apnoea test.

So, how accurate is Sleep Testing Australia overall?
Sleep Testing Australia can be very accurate for identifying likely OSA when the right candidates use a properly fitted home test, and interpretation is handled by qualified professionals. Accuracy is highest when symptoms and risk factors clearly point to a breathing-related sleep disorder, and when they escalate to in-lab testing for complex cases. The best results come from matching the test to the suspected condition, not forcing one test to answer every sleep question. Learn more about is a sleep study Perth worth it for diagnosing sleep disorders?
FAQs (Frequently Asked Questions)
How accurate is Sleep Testing Australia in detecting obstructive sleep apnoea (OSA)?
Sleep Testing Australia is generally very accurate for detecting common sleep disorders like obstructive sleep apnoea (OSA), especially when the test type matches the patient’s symptoms. Accuracy depends on whether an in-lab sleep study or a home sleep test is used, how well sensors capture data overnight, and if a qualified clinician interprets the results in context.
What types of sleep tests does Sleep Testing Australia offer?
Sleep Testing Australia typically provides home sleep apnoea testing (HSAT) designed to detect breathing-related sleep disorders. They may also facilitate in-lab polysomnography through partner clinics or referral pathways, which records more signals and is preferred for complex symptoms or suspected non-breathing sleep disorders.
When should someone opt for an in-lab polysomnography instead of a home sleep test?
An in-lab sleep study is more accurate when measuring detailed parameters like sleep stages, arousals, limb movements, seizures, or unusual behaviors during sleep. It’s recommended for individuals with significant comorbidities, suspected central sleep apnoea, or if prior home testing was negative despite strong symptoms. The additional sensors help reduce ambiguity and confirm diagnoses.
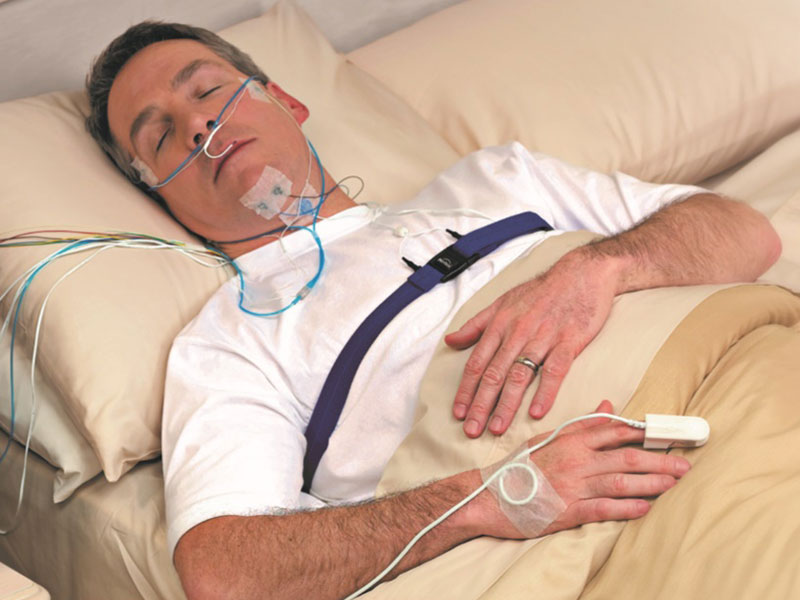
How does sensor placement and user setup affect the accuracy of home sleep tests?
Proper sensor placement and user setup are crucial for accuracy, especially in home tests. Misplaced nasal cannulas, loose oximeters, or improperly positioned chest belts can lead to undercounting breathing events or misreading oxygen levels. To mitigate this, many services provide clear instructions, fit-check guidance, and data-quality screening before finalizing reports.
Can Sleep Testing Australia’s tests miss a real sleep disorder?
Yes, some conditions can be missed if the wrong test is used or if the disorder is intermittent. Mild OSA might go undetected if few events occur during the test night. Some disorders require specialized testing beyond standard apnoea studies. Therefore, normal results should always be interpreted alongside symptoms, medical history, and risk factors.
What steps should be taken if sleep test results do not align with symptoms?
If test outcomes don’t match clinical symptoms, patients should discuss results with a qualified clinician who may recommend repeating the study or conducting an in-lab polysomnography. Reviewing device data quality for artefacts or poor signals is important. For symptoms like severe daytime sleepiness or unusual night behaviors, alternative diagnostic pathways may be necessary beyond home apnoea testing.